Pregnancy Gingivitis Causes and Facts: Keeping Patients Informed
Pregnancy gingivitis is a topic that understandably draws a lot of questions and concerns from dental patients.

At a time where the body is undergoing many changes, and expectant mothers are extremely focused on the health of themselves and their baby, any sign of trouble can set off alarms.
The increase in gum inflammation and underlying gingivitis issues during pregnancy is no myth. Dental professionals know that pregnancy gingivitis is a real phenomenon. But it’s also not generally as concerning as patients experiencing these symptoms might think, so long as they understand what they’re dealing with and how best to navigate the situation.
As a dental professional, you can provide a reassuring voice and guiding hand.
What is pregnancy gingivitis?
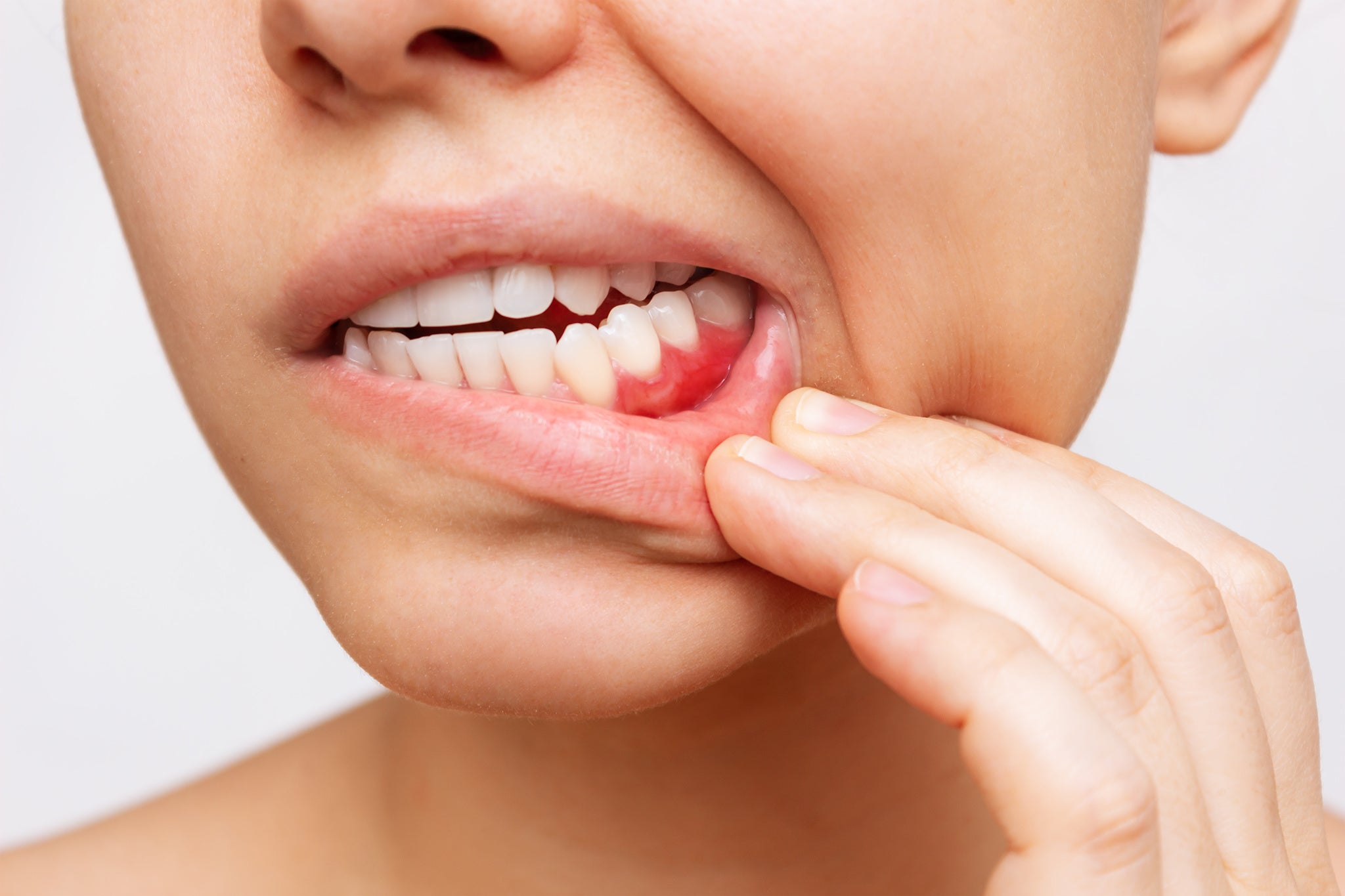
Pregnancy gingivitis refers to the specific condition where inflammation of the gingiva is clearly tied to a woman’s pregnancy. As is the case for “classic” gingivitis, increased bleeding is one of the main symptoms of this condition. Pregnancy gingivitis often first occurs late in the first trimester, and peaks in the eighth month, dissipating shortly after delivery.
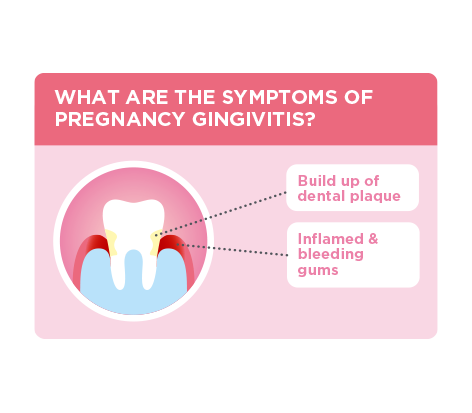
While gingivitis — a precursor to periodontal disease — can affect anyone at any time, the term “pregnancy gingivitis” is distinct because its circumstantial causes and considerations are more nuanced than general instances of gingivitis and gum inflammation.
The most important fact for patients to know is that pregnancy gingivitis is not at all uncommon. Research suggests that this condition affects between 60 and 75% of pregnant women, meaning that an expectant mother is more likely than not to experience it.
At the same time, there is a pervasive lack of awareness around pregnancy gingivitis. A questionnaire in 2019 found that a “Majority of pregnant women were found unaware about developing of pregnancy gingivitis as well as the cause, effects, treatment, and preventive measures for the same.”
With this in mind, it is all the more critical for providers to be proactively equipped with credible information about causes, concerns, and recommendations.
Pregnancy gingivitis causes
As we all know, numerous changes take place within the body during pregnancy. Among them is a steep increase in hormones (specifically progesterone and estrogen).
It is believed that these hormonal changes are the main driver of pregnancy gingivitis by greatly aggravating a disease that already existed before the pregnancy. It is therefore important to note that pregnancy itself doesn’t cause gingivitis. The increased inflammation observed in pregnancy gingivitis can even occur in patients who do not have an increased dental biofilm mass.
However, the mechanisms behind this are not entirely understood. One of the explanations could be that the maternal immune response changes during pregnancy, making them more vulnerable to the host inflammatory response to the bacterial challenge in the dental biofilm. For example, it stimulates the production of cytokines that are involved in the inflammatory response (such as prostaglandins).
Other evidence points towards a shift in the oral microbiome, caused by the hormonal changes.
Whatever the causes are, there are three things to suggest to patients experiencing pregnancy gingivitis:
- It is not necessarily a sign that their oral care has been poor.
- It is not a sign that anything is wrong with their pregnancy.
- It is not a reason for panic, because this is a natural byproduct of complex processes in the human body.
Dental professionals can, however, use this condition as a call-to-action, building additional urgency into the guidance around developing excellent at-home oral care rituals. Ideally these habits will stick long after the happy arrival of a healthy little one.
Preventing pregnancy gingivitis
The measures for preventing and combating pregnancy gingivitis are largely the same as those for preventing general oral health issues. But they take on added emphasis during this very crucial time of bodily change.
If you learn that a patient is pregnant, it may be helpful to walk them through the underlying causes and symptoms of pregnancy gingivitis, while laying out a clear plan for prevention and management. This could include:
- Commitment to at-home oral care rituals. Brush twice a day and practice interdental cleaning regularly. If the patient is already experiencing inflammation and soreness, you may want to help them find an extra-soft toothbrush, while demonstrating gentle techniques.
- Eat a healthy diet. Many expectant mothers are already taking extra care with what they eat and drink, knowing that it affects more than just them. As a dental professional, you can help steer them toward teeth-friendly options like fruits, vegetables, grains, and dairy, while urging minimal intake of sugars, starches, and acids.
- Pay an extra visit to the dentist. While cleaning and checkup visits are typically recommended once every six months or so, it might be worth advising a pregnant woman who is concerned about gingivitis to come in once extra time during the nine-month pregnancy, just for peace of mind. You can examine their gums, regroup on the preventive plan, and offer comforting assurance. To prevent any unnecessary alarm or pressure, frame this as totally optional for the patient.

One other common habit for pregnant women who are experiencing gingivitis is to routinely swish salt water around in the mouth for a few seconds and then spit it out. Sea salt can help reduce inflammation and promote healing.
Additionally, for those women who are experiencing nausea and vomiting as a result of morning sickness, make sure to advise they wait at least 30 minutes after throwing up before brushing, as the acidic content of vomit can pair with abrasives in toothpaste to damage enamel.
Finally, if a pregnant woman suffers from pregnancy gingivitis, or even worse, periodontitis, it is good to know that periodontal treatment is both safe and effective. Research shows that by delivering dental prophylaxis and follow-up oral hygiene instructions, you are able to improve all relevant clinical measurements, such as bleeding and plaque indices, probing pocket depth and clinical attachment loss.
Pregnancy and oral health: More tips and resources
Because pregnancy is a time where people tend to be fervently focused on their health, and during which oral health naturally emerges as a more prominent issue, it’s a key moment of opportunity to cement lifelong routines and rituals for healthy teeth and gums.
For more information concerning pregnancy and the coinciding oral health considerations, here is some additional recommended reading and viewing:
- Our Pregnancy and Oral Health page features information and advice pertaining to pregnancy gingivitis as well as other, less common issues that can emerge, such as pregnancy granuloma and teeth erosion.
- Learning about the Gum Link, and how the health of one’s mouth has a substantial impact on the health of their body, might help pregnant women put even more weight into their at-home care.
- The webinar viewable here (or below) features a 50-minute panel discussion with Dr. Mia Geisinger and Prof. Dr. Phoebus Madianos, who share their insight and expertise on a variety of topics, including the influence of pregnancy on oral health, periodontal implications and treatment during pregnancy, collaboration between dental professionals and the perinatal team, and more.
"Positive behaviour change during pregnancy is really a critical opportunity," said Dr. Geisinger during the webinar.
"Pregnancy has been identified as a time when women are more likely to make those positive behavioural changes, particularly those that will benefit their fetus."
She adds: “If we can take the time to counsel our patients about the benefits of, in particular, self-delivered oral hygiene... that could have a lifelong effect.”
Take a positive perspective, highlight those benefits, and use pregnancy gingivitis as an opportunity to educate and motivate your patients.