Inflammatory periodontal disease: what the science says
Dental professionals recognize that inflammatory processes are at the basis of periodontal disease. However, we’re still learning more about how this exactly works, and the scientific community continues to explore implications and impacts.
It’s important to not only stay up to date on the latest research around this topic, but also to be able to communicate it clearly to your patients. There are two primary reasons for this:
- The first symptoms patients with periodontal issues usually notice are those caused by inflammation, so awareness can help patients vigilantly spot and address emerging concerns early on.
- Understanding the relationship between inflammatory responses and the clinical picture of periodontal disease helps patients understand how periodontal disease can impact their systemic health as well, underscoring the vital importance of a consistent, comprehensive oral care routine.
Inflammation at the basis of periodontal disease
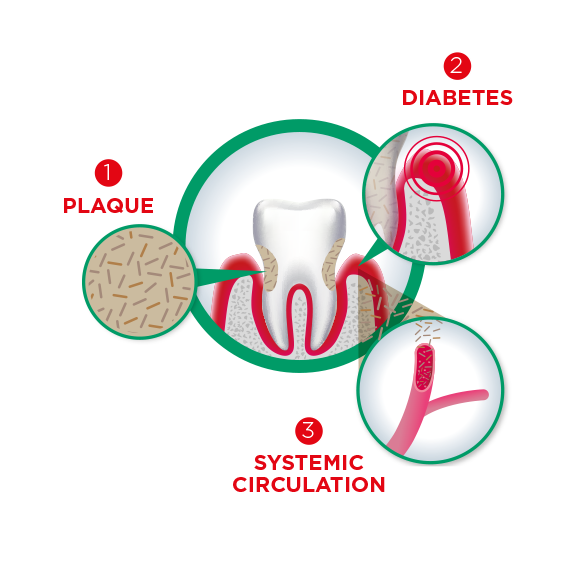
Periodontitis is a chronic inflammatory disease that is caused by a host immune response to the dental biofilm. Plaque accumulation due to poor oral hygiene is one of the major risk factors, as it’s obviously a necessity to elicit an immune response in the first place. In fact, not removing dental plaque on a regular basis will elicit inflammation and cause gingivitis in most people.
However, it has also become obvious that the actual damage to the periodontal tissue is mainly caused by the host response to the pathogens in the biofilm, not the pathogens themselves.
That host response is influenced by several factors, such as genetics, lifestyle, aging, systemic diseases and many more. This also probably explains why some individuals seem to be susceptible, while others demonstrate some sort of protection against periodontal disease.
The initial inflammatory response causes local but reversible damage to the gingival tissue: gingivitis.
At one point, this lesion can progress into periodontitis, in which other structures are being destroyed as well, beyond the point of repair. This switch is sometimes defined as “exacerbation”.
Although still largely hypothetical due to the lack of longitudinal research, it is thought that the inflammation in gingivitis contributes to the development of a dysbiosis: a changing composition of bacterial species towards a more pathogenic biofilm. In turn, this dysbiosis can enhance the inflammatory response even further. The body can respond in two ways: repair or destroy, with the latter one causing the destruction that characterizes periodontitis.
A recent review article by Prof. van Dyke of the Forsyth Institute summarized this principle perfectly: “Whether dysbiosis initiates disease or is a consequence of disease initiation has not been definitively demonstrated, but it is clear that the nexus between inflammation and dysbiosis is critical.”
Explaining periodontal issues to patients through the lens of an inflammatory response can make this extremely complex matter more easily understood, because almost everyone has a basic understanding of how inflammation works as a bodily response to injuries or infections.
Patients understand that our ankle swells up if we sprain it, or that our skin tends to become reddened around a cut.
As mentioned above, the inflammatory response in the gingival tissue that characterizes gingivitis or periodontitis is the cause of some of the earliest symptoms, so encourage your patients to look out for swelling, bleeding, or sensitivity in the gums.
Not only can a clear understanding of inflammatory response equip patients to better spot emerging oral health problems, but it can also accentuate why it is essential to act upon them quickly. Not just for the good of their mouths, but for their holistic health and well-being.
Inflammation, periodontal disease, and systemic health issues
Periodontal disease and the associated inflammation have been scientifically linked to a number of systemic health issues. Research has drawn connections with at least 57 systemic conditions and inflammation-driven disorders, including arthritis, diabetes, and cancer.
Three health issues in particular have risen to the forefront and might be worth calling out specifically with patients:
Links Between Gum Disease and Cardiovascular Disease
Cardiovascular diseases (CVDs) are the leading cause of death globally. There’s a good chance that many of your patients know or love someone who has been affected by this terrible affliction. Many are probably not aware of a link between cardiovascular disease, specifically atherosclerotic cardiovascular diseases (ACVDs), and inflammatory periodontal issues.
Based on research findings, the European Federation of Periodontology concludes that, “There is evidence that periodontitis is associated with various forms of cardiovascular disease, including:
- Coronary artery disease
- Myocardial infarction
- Cerebrovascular disease
- Cardioembolic and thrombotic stroke
- Peripheral artery disease
- Atrial fibrillation
- Heart failure.”
Research shared by EFP finds that:
- Patients who brush their teeth less than once a day have the highest incidence of acute CVD events.
- Patients who brush their teeth twice a day and have a good oral-health routine may reduce the incidence of acute CVD events.
- Successful periodontal treatment could reduce the incidence of acute CVD events independently of traditional CVD risk factors.
In light of these insights, “It is therefore very important to maintain a good oral-health hygiene with a daily routine of brushing teeth twice a day, cleaning between the teeth (interdental cleaning), visiting the dentist regularly, and having any gum disease treated.”
Pregnancy Gingivitis and Concerns for Expectant Mothers
When expecting a child, women tend to naturally become extra-vigilant about their health, for reasons that require no explanation. Because of this, the common occurrence of pregnancy gingivitis, which can affect 60-75% of pregnant women, presents an opportunity to emphasize the urgency of oral care routines.
In short, this condition refers to increased inflammation in the gingiva as a direct byproduct of a woman’s pregnancy. Causes of pregnancy gingivitis are not fully understood, but may relate to maternal immune response changes due to hormonal changes during pregnancy.
“The clinical studies we performed at Chapel Hill show that fetuses that had an antibody response against periodontal pathogens had a much higher chance of being born prematurely or at low birth weight,” explained prof. dr. Phoebus Madianos in a recent SUNSTAR Conversations PRO webinar. “This implicates that bacteria can travel from the periodontal pocket and even reach the fetal-placental unit, eliciting local inflammatory reactions or even infecting the fetus directly.” As we’ve shared in the past, pregnancy gingivitis is not something to be overly worried about on its own. But it may be a scenario in which you can clearly draw out the deeper connection between oral health and other parts of the body, while giving patients increased motivation to double down on their home oral care habits.
“There has been a paradigm shift,” according to prof. dr. Mia Geisinger. “A few decades ago, when a woman got pregnant, she was told by her dentist: see you in 9 months. While we know now that oral care is critically important.”
Watch the full expert discussion below:
Periodontal disease and obesity
The relationship between periodontitis and obesity is one that has been gaining a lot of attention from medical research communities. A recent issue of Periodontology 2000 shares that, “Epidemiologic evidence from the last 2 decades has established an increase in periodontitis prevalence in obese and overweight individuals. Biologic mechanisms potentially linking obesity and periodontal disease are adiposity-associated hyperinflammation, microbial dysbiosis, altered immune response, specific genetic polymorphisms, and increased stress.”
"Periodontal disease occurs in patients more susceptible to inflammation who are also more susceptible to obesity,” said Andres Pinto, professor of oral and maxillofacial medicine and diagnostic sciences at the Case Western Reserve University School of Dental Medicine. “Oral health-care professionals need to be aware of the complexity of obesity to counsel their patients about the importance of an appropriate body weight and maintaining good oral hygiene."
Another recent study shows that obesity raises the risk of gum disease by inflating growth of bone-destroying cells and increasing alveolar bone destruction, providing a more detailed mechanistic appreciation of the interconnection between obesity and periodontitis.
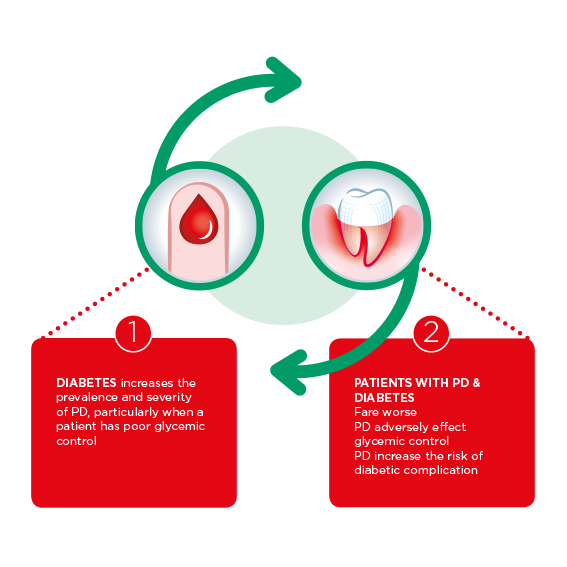
Of course, obesity is also strongly linked to diabetes, which itself has been connected to periodontal disease through significant scientific evidence.
This relationship has been known for some time, and is worth bringing up with patients as another example of how oral health can impact holistic health and vice versa.
Keep yourself and your patients informed
Every dental professional aspires to help their patients avoid letting oral health issues advance to the stage of periodontal disease. We all know that embedding strong oral care rituals is the most effective way to do so, but different people respond to different messages and motivators.
Understanding the latest science around inflammation and periodontal disease, and communicating it to patients in a clear and compelling way, can play a role in framing the importance and impact of their at-home care. The bottom line is that an inflammatory response is our body’s way of telling us something is wrong, and that’s a prompt to take action.
For patients who are already experiencing inflamed or bleeding gums, you might consider recommending GUM® PAROEX® 0,12% Intensive Action Mouthwash, which can address existing plaque while also preventing further problems from appearing by stopping new plaque from building up.
This mouthwash also helps soothe sensitive gums.