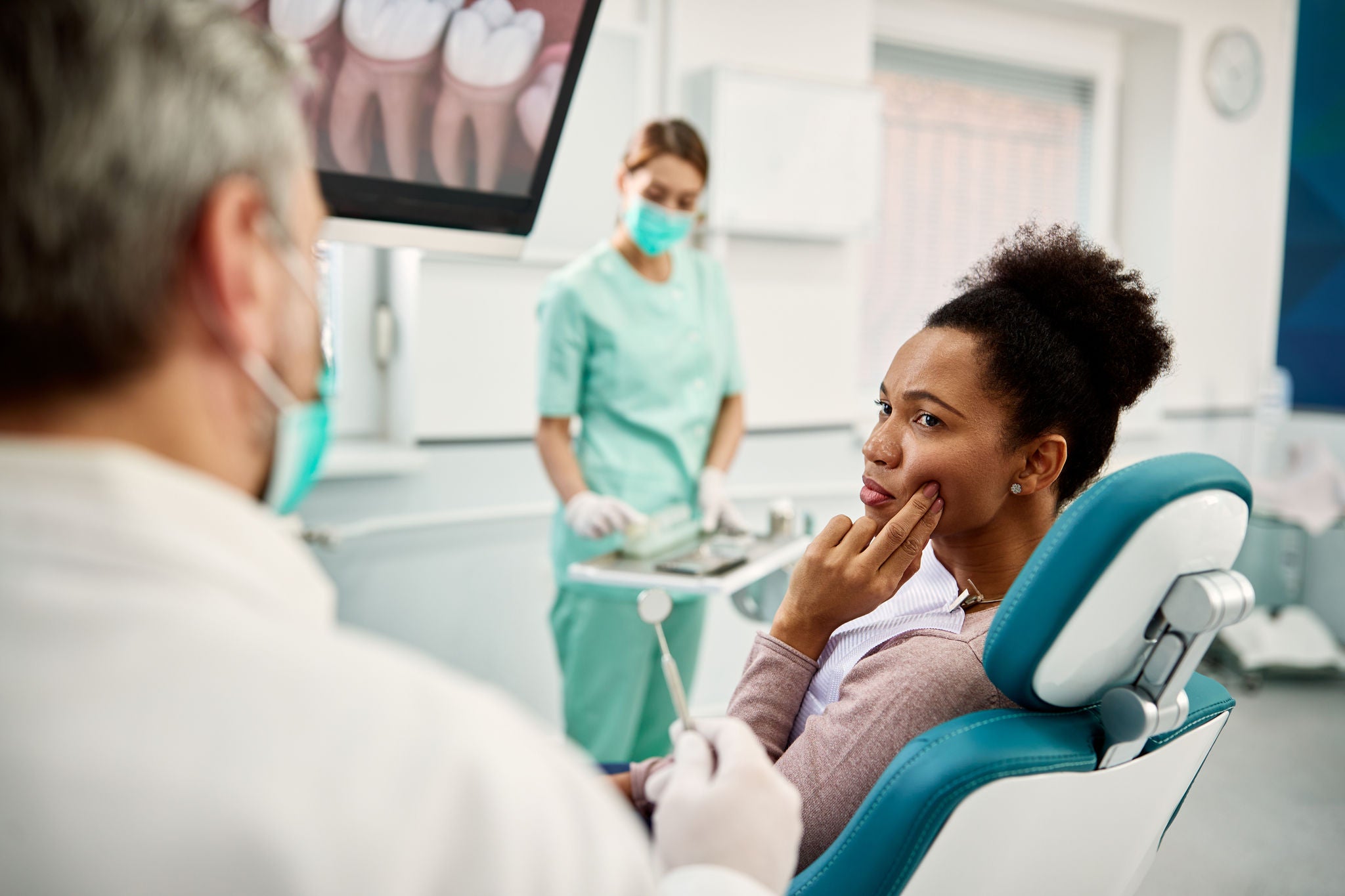
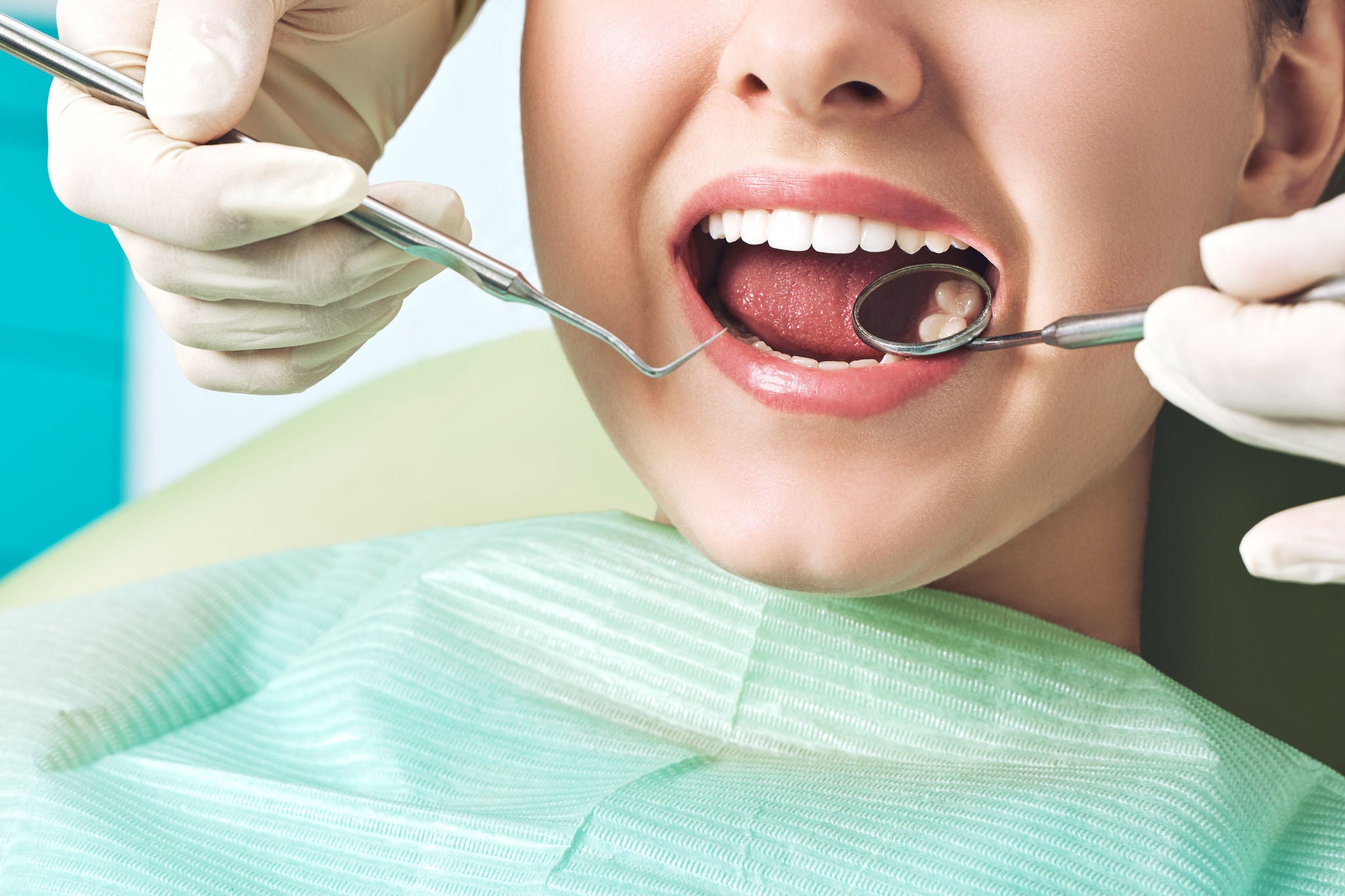
Advising Patients on Links Between Diabetes and Periodontitis
As a dental professional, you are probably aware of the complex bidirectional relationship between diabetes mellitus and periodontitis. However, for everyday people, it is not always clear that such a connection exists. As a result, patients might view their oral hygiene habits as a necessary evil to prevent oral health issues, while in the meantime, missing the point that good oral health can also have extended health benefits.

This is a challenge for dental professionals. How do you communicate with your patients about the complex relationship between diabetes and periodontitis without confusing or scaring them? It’s all about connecting the dots in a comprehensive and meaningful way.
Helping Patients Understand the Relationship Between Oral Health and Overall Health
The first hurdle is explaining oral hygiene as part of total health. What happens to the rest of your body if you neglect a single part? Use relatable examples to make your point. If your diet is poor, it affects your sleep. If you don’t sleep well, it affects your mood. The point is rather simple: every aspect of your health affects other ones in some way.
The link between periodontitis and diabetes [1] is no different. Make it clear that neglecting the mouth means neglecting the body. Oral hygiene is part of general health in the same way sleep, diet, skin care, and exercise are.
Conveying the Consequences of Insufficient Dental Care
Establishing oral health as part of overall health is only effective when you show the consequences. Aside from cavities and bad breath, what happens when you don’t brush your teeth and clean between them appropriately? Discuss with patients the role of bacteria that are present in their dental plaque, and the many problems they could contribute to, such as:
- Cardiovascular disease: Those with gum disease have a 2-3x higher risk [2] of having a heart attack, stroke, or similar cardiac event, although here is no proof of a direct connection.
- Endocarditis: The link between infective endocarditis and oral bacteria has been known for decades [3].
- Pneumonia: There is an established relationship [4] between gum disease and bacterial pneumonia, with anaerobic bacteria in dental plaque considered a logical contributor.
- Respiratory infections: Studies have shown [5] that gum disease may increase the risk of respiratory infections other than pneumonia, like COPD.
Your patients need real examples with real consequences to show how the simple acts of brushing and interdental cleaning profoundly (and positively) impact wellness. Frame the severity of poor dental hygiene through the lens of its effects.
Positioning Periodontitis as a Serious Health Issue
The numbers speak for themselves. Periodontal disease statistics are staggering [6]. It’s estimated that approximately 80% of people over age 30 have some form of periodontal disease - from mild gingivitis to periodontitis. In real numbers, that’s 750 million people worldwide. Delving deeper, severe periodontitis affects as many as 10–15% of adults [7]. Juxtapose these figures with the number of estimated cases of diabetes worldwide (415 million) [8] and it’s clear to see how significant the problems posed by these two chronic diseases are.
People living with diabetes are 1.5-3 times more likely [9] to suffer from periodontitis than people without. The data points to an irrefutable link. This emphasizes why it is even more important for patients with diabetes to take preventive measures, which can potentially help with avoiding health hardships. Evidence suggests gum disease may worsen the complications of type 2 diabetes [10].
Periodontitis and Diabetes
Research suggests a complex bidirectional relationship [11] between periodontitis and diabetes. Diabetes is a major risk factor for periodontitis, and studies have established a clear link between the degree of hyperglycemia (high glucose levels) and severity of gum disease. Those with diabetes (type 1 or 2) are more likely to experience other unpleasant oral health issues such as bad breath, dry mouth, oral infections, and aggravation of periodontal disease.
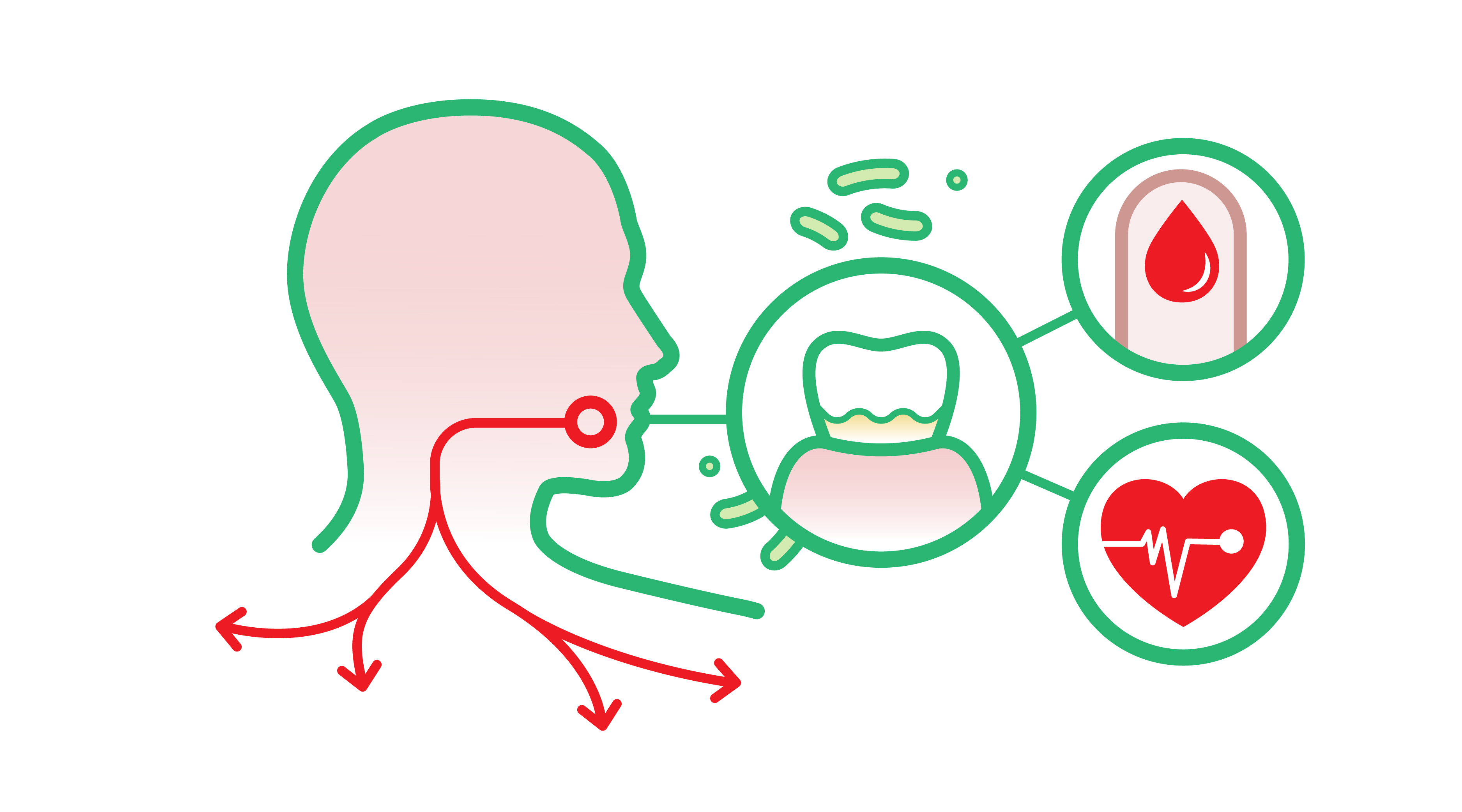
Meanwhile, periodontitis can have a negative impact on glycemic control of patients with diabetes, meaning it can be increasingly difficult to maintain steady blood glucose levels. This in turn increases the risk for (severe) diabetes complications with - for example - the eyes, kidneys and nerves. This is obviously a pertinent point to present for any patients who may have diabetes, or are at risk for it. But it also serves to more generally reinforce the whole principle of complete health.
Remember, as a dental professional, it's not about what you know; it's about what you can help stick in the minds of your patients after they leave your chair.
Preventive Steps to Recommend
No education is complete without homework—takeaways that keep the lesson fresh and build on the concepts learned. Teaching patients about the links between periodontitis and diabetes necessitates a checklist. Pass these easy-to-remember, easy-to-do items off as routine and encourage all patients - especially at-risk ones - to follow them:
- Practice interdental care, cleaning between teeth to remove plaque and stimulate gums.
- Brush regularly, twice each day or after every meal for at least two minutes, to prevent plaque buildup.
- Rinse after brushing using a gentle rinse or mouthwash to remove harmful bacteria.
- Schedule regular dental checkups biannually or quarterly for cleaning and care.
- If you are familiar with diabetes mellitus, ensure that you are up-to-date in terms of metabolic control.
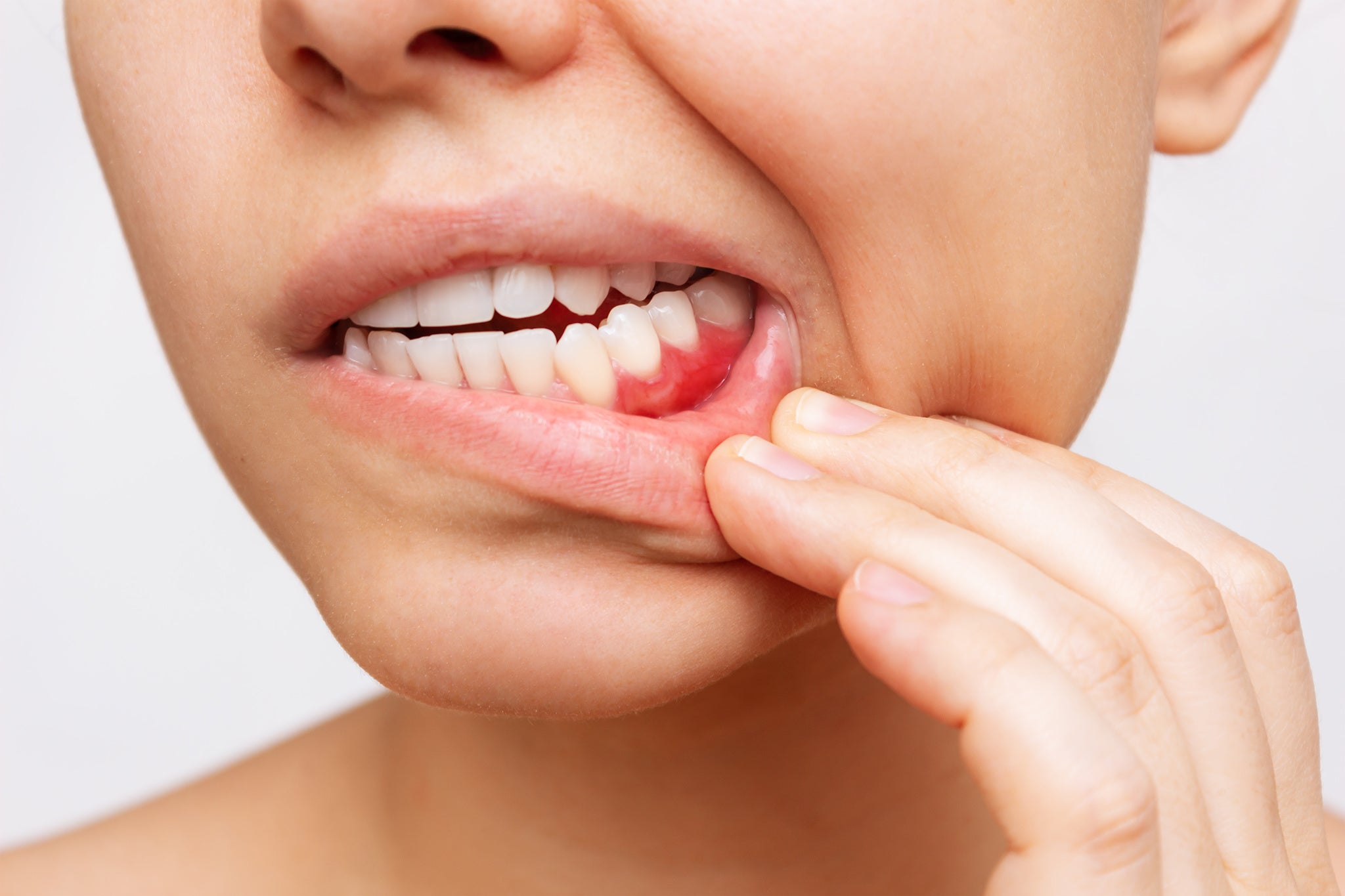
- Familiarize yourself with signs of gingivitis and periodontal disease, such as bleeding after brushing.
- Be mindful of the links between oral hygiene and overall health and wellness.
Helping patients understand the links between gum disease and diabetes requires broader conversations about oral hygiene and total wellness. It needs to be part of an ongoing approach to dental education, made simple for patients to comprehend and take seriously.
We invite you to learn more about the bidirectional link between periodontitis and gum disease, and also to learn more about SUNSTAR GUM® products and how to give your patients the best guidance possible!