Interdental Oral Hygiene: Navigate the Evidence with Ease
In our ever-connected world, oral health professionals may be expected to keep up with advancements in dental research and clinical recommendations. After all, many of our patients have ready access to all kinds of information online and may well use it before coming to consult us about their oral health.
Indeed, it is common for all of us to use online resources for a quick search to prepare for an upcoming discussion, dental visit or meeting. Although online information is a great resource, dentists agree, it is often difficult to evaluate the extensive literature available in terms of validity, quality of data, and reliability of information [1].
How can we keep track of so many publications and so much data?
One thing is for sure: it’s not easy.

Evidence yes, but how much evidence?
Evidence in the healthcare world is exploding, and dentistry is no different. Consider a couple of “fun facts” about the growing body of evidence:
- A team in the US estimated that, in order to keep up with the 7’827 relevant articles published monthly, a family medicine physician would need to dedicate 627.5 hours to reading the medical literature each month, equivalent to 21 hours per day [2].
- A PLoS One publication found that the total number of dental journals increased significantly from 46 in 2003 to 83 in 2012 [3] But that was 2012!
- Today there are more than 100 dental journals [4] and some 26 dental hygiene journals [5].
- How to keep up? How do we deal with an explosion of available medical literature? Just not possible you may say…

In come evidence-based summaries of the literature updating us on what the latest peer-reviewed, published evidence suggests. These come in many forms, from a review of takeaway messages and conclusions of key studies, such as in White Papers, to highly protocolized systematic reviews with complex statistical analysis, gold standard among which are the highly respected Cochrane library reviews [6] that combine the results of only the best quality studies, i.e. randomized controlled trials.
This approach to the reduction of complexity has become an invaluable resource in the current dynamic world of ever-exploding data, essential for us to keep up as knowledge and evidence expand over time.
So, what is evidence-based medicine or EBM all about? Let’s take a closer look.
Evidence-based medicine (EBM) and evidence-based dentistry (EBD)
The British Medical Journal (BMJ) was one of the first to describe evidence-based medicine (EBM) and defined it as “the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients“ [7].
What about dentistry? The American Dental Association (ADA) defines “evidence-based dentistry (EBD),” as an approach to oral health care that combines systematic assessments of clinically relevant evidence, with clinical expertise and the patient's treatment needs and preferences [8].
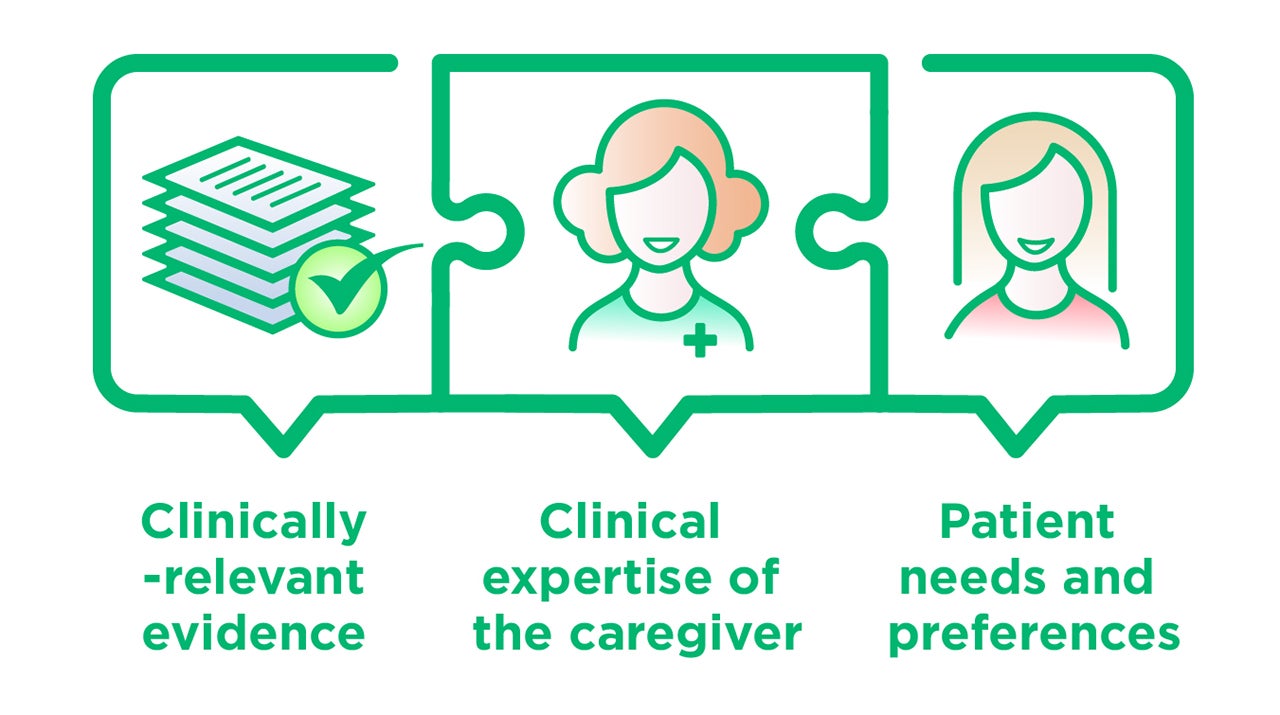
In adopting this definition, the ADA recognizes that, while yes, treatment recommendations can be guided by the evidence, in the end, the final recommendation should be determined for each patient by his or her caregiver, and that patient preferences should be considered in all decisions [8].
It would seem then, that evidence-based medicine is something that helps us navigate a sea of information, summarising what’s out there, helping us to make sense of it all.
Interdental oral hygiene (IOH) to prevent and treat gum disease: so, what is the state of the evidence here?
As you know, a wide assortment of mechanical interdental cleaning devices is available fitting an array of habits, preference and interdental spaces. This assortment includes floss, interdental brushes (IDBs) and rubber interdental cleaners (RICs), all of which are effective when used correctly.
But what if you want to know more about the relative performance of these cleaning devices? What does the latest literature say for each of these interdental cleaning approaches? Which ones are more likely to drive compliance? How can you use this information to guide and indeed simplify your recommendations and adapt them to each patient?
In order to make evidence-based patient recommendations, we need of course to take a look at the latest evidence from the literature. Do you have time to read some 20 lengthy papers comparing IOH devices in prevention and treatment patients?
Well, we did that for you! We performed a literature review entitled “Interdental cleaning to prevent and treat gum disease: state of the evidence” [9]. We looked at 17 randomized controlled trials, and 6 systematic reviews and meta-analyses selected because they compared the efficacy of floss, IDBs and RICs at controlling plaque. We did this for prevention in orally healthy individuals, as well as for treatment in patients with gingivitis or periodontitis.
To learn more about what the latest oral hygiene literature says about floss, IDBs and RICs, download our white paper.

You can also view our Virtual Training, Module 1 “Interdental Cleaning: state of the evidence” which includes interviews of Prof. Graziani.
“Summarising the evidence helps bridge the gap between doctors and patients”, says Mariano Sanz
The Federation of Periodontology (EFP) has also just completed an extensive review of the literature on the treatment of Periodontitis and has – for the first time in its history – published formal evidence-based guidelines for treating Periodontitis [10].
This was a lengthy and painstaking exercise completed in a 2019 Perio Workshop attended by 90 experts from 19 countries. They synthetized the evidence from 15 systematic reviews of current evidence on the treatment and prevention of Periodontitis.
The EFP’s idea is for these guidelines to offer oral healthcare professionals therapeutic pathways based on individual patient diagnoses. The intent is to help oral health practitioners all over the world provide the best possible treatment to their patients, facilitating the adoption of the most appropriate preventive and therapeutic interventions depending on the stage and grade of Periodontitis.
"This guideline will ultimately benefit the patient who would receive the best possiblentreatment under its provisions,” said Mariano Sanz, who chaired Perio Workshop 2019 which developed and published the guidelines [11].

Evidence-based dentistry for peace of mind
In summary, in a world of ever-greater data studies and publications, summaries of the literature, evidence-based dentistry (EBD) and clinical practice guidelines (CPG) based on that summarized evidence, help us navigate complexity. They give us peace of mind that we are doing the best for our patients.

Summarized evidence does not dictate our decisions, nor does it lock us in. Each patient is different, with his or her own fears, preferences and expectations. But it does help us by guiding our recommendations for each patient type, looking at the level of evidence so that we know the “latest baseline” as we make our clinical decision.
So, when you want to know the latest or are unsure, save time. Refer to summaries of the evidence, and if available, check out clinical practice guidelines!
[1] Vineet Dhar “Evidence-based dentistry: An overview“ Contemp Clin Dent. 2016 Jul-Sep; 7(3): 293–294.
[2] Alper BS, Hand JA, Elliott SG, Kinkade S, Hauan MJ, Onion DK, Sklar BM. “How much effort is needed to keep up with the literature relevant for primary care?” J Med Libr Assoc. 2004 Oct;92(4):429-37.
[3] Yasas Shri Nalaka Jayaratne & Roger Arthur Zwahlen “The Evolution of Dental Journals from 2003 to 2012: A Bibliometric Analysis“ PLoS One. 2015; 10(3): e0119503.
[4] https://en.wikipedia.org/wiki/List_of_dental_journals
[5] https://www.omicsonline.org/dental-hygiene.php
[6] https://www.cochranelibrary.com/ and https://www.cochranelibrary.com/cdsr/reviews.
[7] Sackett D, Rosenberg W, Gray J, Haynes R, Richardson W. “Evidence based medicine: what it is and what it isn’t. “ BMJ 1996; 312:71-2.
[8] ADA Policy on Evidence-Based Dentistry, ADA website, Updated: August 29, 2013.
[9] “Interdental cleaning to prevent and treat gum disease: state of the evidence“ An Oral Health White Paper Series | N°2, © Sunstar Europe Sàrl Sunstar Professional, version2, Feb 2020.
[10] Sanz M, Herrera D, Kebschull M, et al; On behalf of the EFP Workshop Participants and Methodological Consultants. “Treatment of stage I–III periodontitis—The EFP S3 level clinical practice guideline”. J Clin Periodontol. 2020;47:4–60.
[11] Perio Insight 13 - Summer 2020 “EFP publishes first evidence-based treatment guidelines for periodontitis”.