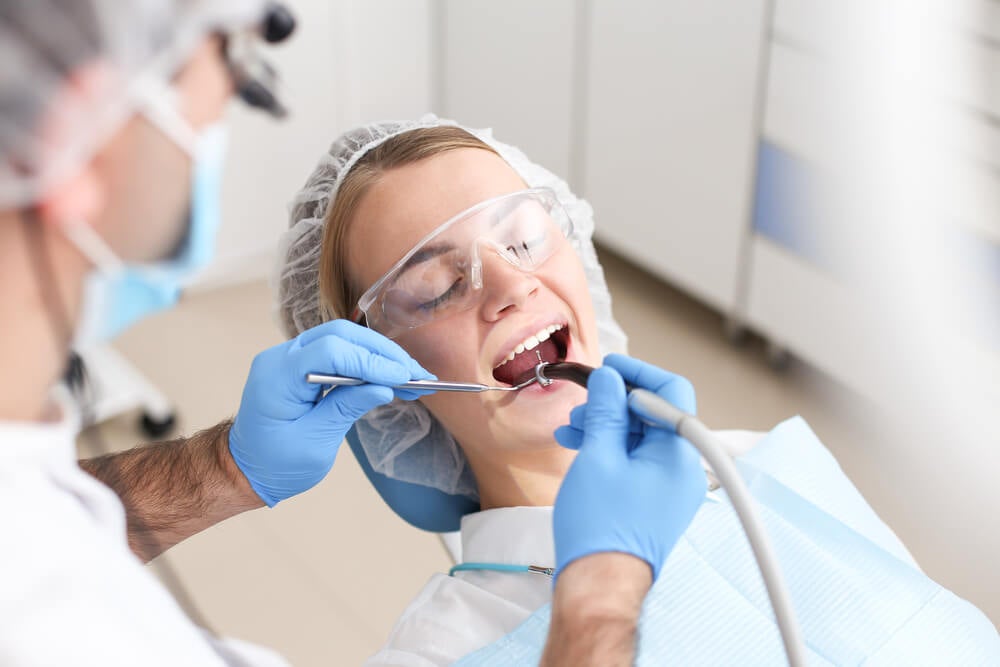
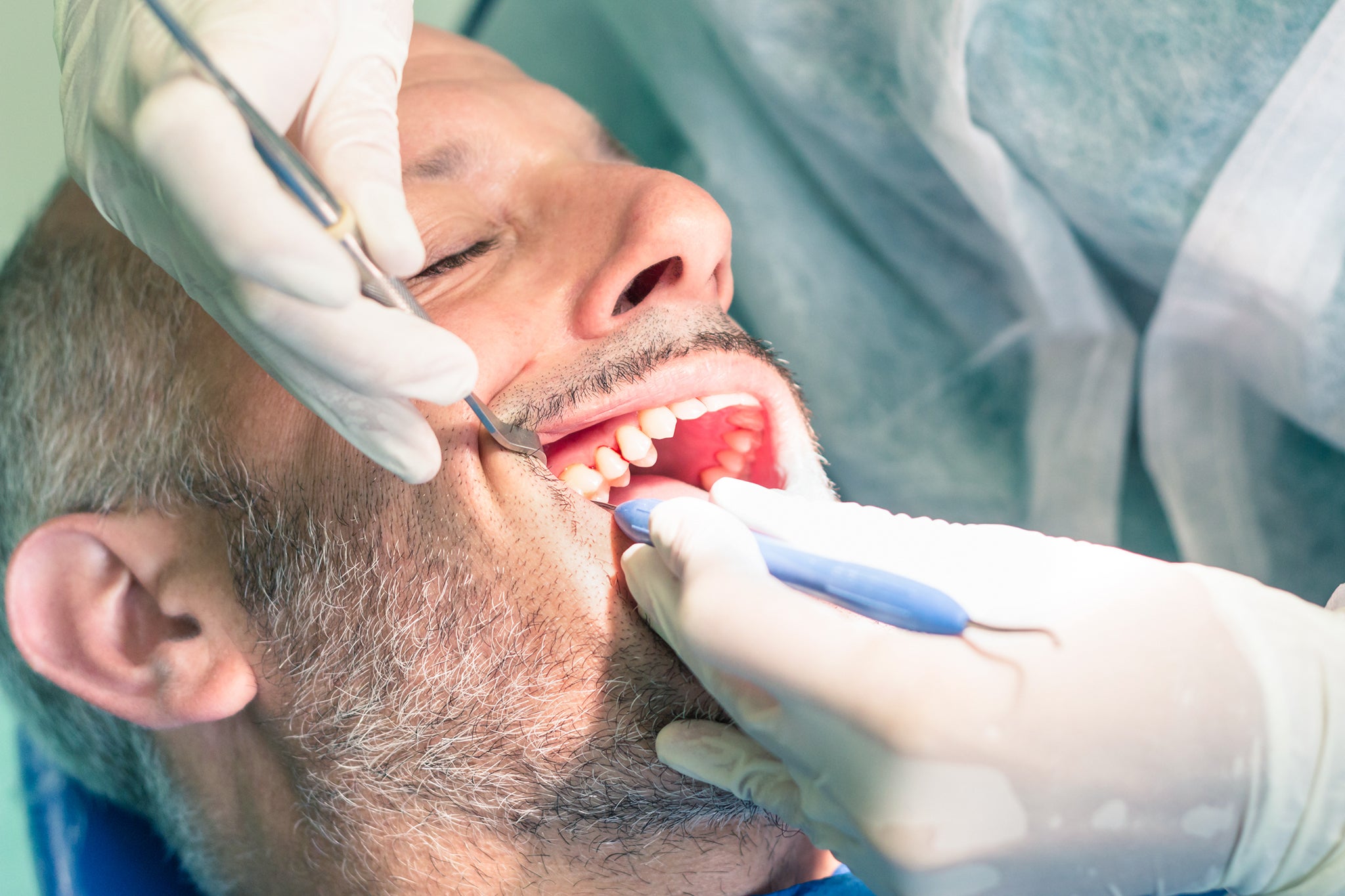
How Dentists Can Drive Behavioural Change in Patients
The old adage “success breeds success” is true for the dental practitioner as well as for the patient.

Dental care which includes targeted positive improvements in your patients’ at-home oral health care creates the benefit of enhanced overall health. Importantly for you, the dentist, behavioural change strategies can be a win for everyone. The research and science that brought enormous technological changes to dental procedures have been preparing dentists for the increasing emphasis on prevention.
An important aspect in the prevention of the two major oral diseases – dental caries and periodontal disease – includes effective plaque control. Obviously, this also requires effective self-performed oral hygiene from your patients. Unfortunately, compared to the theoretical straightforwardness of most preventive strategies, their practical application is often difficult and not always successful. One of the biggest challenges is modifying human behaviour. Studies on the various aspects of habit modification can enlighten dentists to motivate their patients to adopt home care practices that help prevent oral and systemic diseases. Accomplishing this goal requires knowledge in how to create behavioural change in others.
Know Your Challenges
Dentists rarely perform procedures in ideal situations; challenges are commonplace. The hyperactive tongue, excess saliva, inadequate anaesthesia, and limited opening are familiar barriers to overcome to deliver excellent dental treatment. Changing your patient's oral hygiene behaviour also faces formidable challenges. Experts in behaviour change emphasize the importance of understanding these factors that hinder successful change.
Common barriers dentists face in motivating patients to adopt healthy oral hygiene habits include:
- Impatience. Most behaviour change does not occur instantaneously but gradually. The lack of instant gratification can hinder both the dentist and the patient. The dentist may expect the patient to act immediately on oral hygiene instructions. The patient expects bleeding gums to resolve as soon as they start their new routine. But the results of changing behaviour requires patience by both parties.
- Attitudes. You have all the information your patient needs for having healthy teeth and gums. Unfortunately, your patient's family and friends' attitudes can present a powerful obstacle to creating healthy habits — but they can also be key allies in affecting change. For patients who are influenced by those around them, family and friends as “partners in crime” may be the push they need to embrace new habits. Consider addressing them as part of your plan.
- Fear. The setting in which you attempt to influence a patient's behaviour creates anxiety for some people. Taking necessary measures to mitigate this fear can help your patient obtain the confidence to make positive changes. Consider discussing next steps at the front desk while finishing up an appointment, rather than while the patient is reclined in a dental chair. Always speak with empathy and at eye-level with the patient.
Know Your Patient
Identify Your Patient’s Profile
There are two modes of cognitive control — proactive and reactive. This relates to the process by which someone processes information and initiates an action in service of a mental or behavioural goal. A proactive person is motivated by having a specific goal, while a reactive person is more motivated if they have their family and/or friends joining and supporting the new protocol. For greater success in motivating your patient to adopt and maintain new habits, it is helpful to know which type of individual they are. During a recent webinar hosted by SUNSTAR, another way of profiling a patient was proposed by Prof. Newton, a leading expert in the field of behaviour change. He usually classifies people as empathic versus problem solvers. While this can be applied to identify your own personality as a dental professional, it certainly also applies to the patient in front of you. Is he or she a person looking for empathy? Or does he or she wants a solution, without further ado? Knowing and profiling your patient truly is the crucial first step in modifying behaviour.
Create a Comfortable, Respectful, and Supportive Environment
Modifying your patient's behaviour begins the moment you meet. A warm greeting at eye level costs no time from your busy schedule. However, this simple action shows respect, quickly engages your patient, begins to build rapport, establishes trust, and helps forge a relationship that allows you to affect positive change in their life.
Creating this comfortable environment has several effects on your relationship with your patient.
- The patient has a sense of equality between the patient and the dentist.
- The patient has a sense of control and confidence.
- The patient begins to understand that they have a role in their oral health.
- This has the potential to spark the intrinsic motivation necessary to produce habits such as interdental cleaning.
Within this comfortable environment, you now can demonstrate a sincere concern for and interest in your patient as a person. You help them see themselves as the expert in their own oral health. As they start to take ownership of their oral health, even if slightly, you have their attention to transfer helpful oral hygiene information to them.
Know Your Message
The moment you begin your clinical assessment, you begin to convey your message to your patient. Based on your interaction thus far and your clinical findings, you decide how to begin your discussion of:
- The importance of toothbrushing and interdental cleaning.
- The relationship between oral health and systemic health.
- The habits necessary for optimal oral hygiene.
What may not be apparent is how prepared your patient is to receive your message. The TransTheoretical Model (TTM) of behaviour change can help you tailor your message to match your patient’s readiness more precisely for adopting healthy oral hygiene habits.
The TTM stages of change are:
- Precontemplation: The patient is not ready and may be unaware of their need to change.
TIPS: Encourage your patient to re-evaluate their current habits and engage in self-exploration first (rather than immediate action). Explain to them, in a personalized way, the risks of continuing their current behaviour. For example, if they don’t practice good oral hygiene at home, they may require more invasive dental treatments to address cavities and other problems.
- Contemplation: The patient is thinking about changing and is more aware of the benefits of changing.
TIPS: Encourage your patient to evaluate the pros and cons of making a behavioural change in their oral hygiene practices. Identify and promote positive outcomes, such as feeling more self-confidence due to a healthy mouth, having better overall health in later life and being less fearful of dentist visits.
- Preparation: The patient is planning to change and is taking small steps toward action.
TIPS: Help the patient to identify and overcome obstacles to change. Identify people who can support them. Ensure that they have the skills to bring about behavioural change. Encourage them to make small initial steps.
- Action: The patient is changing habits. Teaching the proper oral hygiene techniques is important during this stage.
TIPS: Restructure cues (signals that have significance to the person) and social support (assistance from others) to reinforce positive messages for oral health. Bolster your patient’s self-efficacy (their own judgement of how well they can cope with a situation based on their skills and circumstances). Fight any feelings of loss and remind them of long-term benefits.
- Maintenance: The patient is achieving results with a new routine and is considering how to prevent relapse.
TIPS: Encourage them to find additional support. Point out internal rewards (physical and mental outcomes of the changed behaviour). This might include having a brighter smile, feeling more confident around others, sleeping better due to lack of discomfort and being in better overall health.
Discuss how they can avoid relapsing into old habits, such as writing notes to themselves as daily reminders to brush and floss teeth. Teach them how to deal with “triggers.” In the case of oral hygiene, a trigger may be snacks at work, and the solution may be to bring a toothbrush with them for a quick cleaning during the day.
You can more effectively communicate your message of brushing twice daily and cleaning interdentally daily by combining the TTM with another model, the Health Belief Model. Getting your patient to act based on the information you provide depends on whether:
- The patient believes that a negative health condition can be avoided.
- The patient has an expectation that a recommended action results in the avoidance of disease.
- The patient is convinced that it is possible to succeed in taking action.
These two models are interrelated and can help you deliver your oral health message clearly, timely, and effectively. Keep in mind that your message will need to be “customized” for proactive and reactive individuals.
There are many techniques to help you get your message across more effectively. See “Why Strong Communication Skills Are Essential for Today’s Dental Professionals” for helpful tips on how to successfully communicate with your patients.
Know Your Plan
As dentists' awareness increases regarding the link between oral health and serious medical issues, so does the understanding of the urgent need for patients to change. This requires dental professionals to shift from focusing on treatment to coaching patients to improve their oral hygiene habits.
This includes building rapport, communicating a precise oral health message, and helping patients choose the right products to improve their oral health.
For more help on how you can help your patients improve their oral hygiene and overall health, contact SUNSTAR GUM®.